Previous Article
News
Part 2 | Beyond Rehabilitation: The Power of Nervous System Awareness in Probation
In this three-part series, I advocate for greater nervous system awareness by Probation Officers when working with people on Probation. In this article, I provide an overview of attachment, interpersonal neurobiology, polyvagal theory and state-dependent functioning with reference to offending behaviour.
article written by: Jane Mulcahy, PhD, Research Fellow on the Greentown Project, Research Evidence into Policy Programmes and Practice (REPPP) at the University of Limerick.
In this three-part series, I advocate for greater nervous system awareness by Probation Officers when working with people on Probation. In this article, I provide an overview of attachment, interpersonal neurobiology, polyvagal theory and state-dependent functioning with reference to offending behaviour.
I have written elsewhere that the Risk-Needs-Responsivity (RNR) model, discussed in part 1, completely ignores the relevance of “the dose of interpersonal and developmental trauma to which the offender was exposed”, nor does it appreciate “the fact that learning is impaired if a person is in a state of emotional dysregulation caused by toxic stress and fear.”[1] The RNR model, and indeed desistance theory, fail to grapple with the influence of fear, autonomic dysregulation and involuntary survival responses in undermining a person’s desire for a better, non-criminal future.
Interviews with 12 long sentence male prisoners subject to post-release supervision by the Irish Probation Service as part of my PhD revealed how seemingly disconnected matters such as safety, health, relational capacity, self-perception, behaviour, coping strategies, social stressors, criminality, meaning-making and the ability to feel hopeful about the future were all intimately connected.[2]
Interpersonal neurobiology is the term Siegel coined to explain that our brains and minds are shaped by our relationships and environmental experiences.[3] The human brain – a profoundly social organ – develops from the bottom up. Sensory information first enters the lower, survival-oriented parts of the brain. [4] The emotional, attachment-focused limbic system and the rational pre-frontal cortex, which develop after birth, are highly “experience dependent”.[5]

There is insufficient awareness among criminal justice agency staff, including Probation Officers, that an individual’s safety, relational health, learning ability, impulse control and capacity to be a productive member of society in adulthood begins with the quality of their preverbal attachment experiences. Ludy-Dobson and Perry describe relational health as “the presence, quality, and number of relational supports” that a person has. Relational health during childhood is the ultimate protective factor.[6]
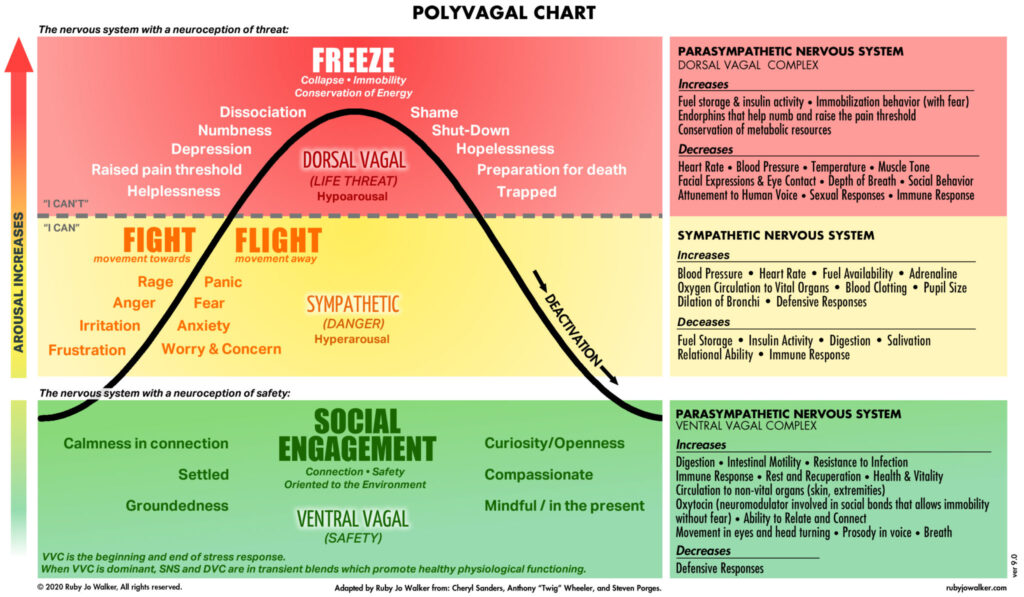
Criminological studies have traditionally neglected the importance of attachment and safety in the first 1,000 days of a child’s life. Polyvagal theory is a science of safety, connection and trust.[7] Porges argues that human bodies are on a quest for safety. Humans are biologically programmed to connect and collaborate with others to survive. When we are in a state of physiological safety, we can access higher cortical functions, whereas when we feel endangered involuntary defensive responses dominate. Neuroception is a process whereby our nervous system unconsciously detects safety or threat in our environment.[8]
A “felt sense”[9] of physiological safety is a prerequisite for flourishing, without which we cannot enjoy physical and mental health, develop reciprocal relationships or adopt pro-social behaviours. Our relational ability, openness to learning new things and our behaviour change depending on the state of our nervous system. Perry refers to this as “state-dependent functioning”.[10] As we become swamped with fear and preoccupied with survival, our IQ drops significantly.
A person’s enjoyment of an embodied feeling of safety in the presence of others starts at birth, becoming contingent on the presence or absence of nurturant care and safety they experience within their family. The first unit of the group, or the wider societal pack, is the family. As noted by Andrews and Bonta, “the family is the child’s first socializing agent.”[11] Our first primal human bond is usually with our birth mother.
Secure attachment establishes the building blocks for future relational health.[12] During the first year of life, babies need to be frequently held and cuddled by their mother, or another warm, loving, consistent caregiver. This ensures survival first and foremost, as well as physical health, optimal weight gain and the development of empathy, trust and pleasure in human connection.[13]
The infant’s mother is often their main, or only, source of potential safety and comfort. A major quandary arises for an infant if their only recourse to seeking safety and comfort is from a frightened and/or frightening source.[14] An unsafe, unreliable, relentlessly or traumatically stressed caregiver cannot give an infant what s/he needs to thrive. This is of great relevance to the backgrounds of offenders, since many come from female-headed households with non-existent, or grossly inadequate paternal buffering.[15]
Unless infants get responsive, sensory-enriched care, they are unlikely to experience normal physical or emotional development. In the first year of life pure neglect (meeting physical needs such as feeding and attending to basic hygiene but failing to attend to the baby’s visceral needs for touch and nurturance) leads to serious neurobiological harm, including empathy deficits that are hard to remedy down the road.[16]
The importance of attachment has been bolstered by recent neuroscience developments.[17] In 2019, research found that perinatal developmental experiences (0-2 months) were more strongly associated with impaired child functioning than adverse experiences occurring during later developmental periods. Moreover, impoverished relational experience during the perinatal period – i.e. poor attachment – was a stronger predictor of negative outcomes than adversity.[18]
Attachment theory sheds light on the barriers that people may have coping with stressors or making sense of interpersonal trauma in their lives. Exposure to overwhelming stress in infancy means that the neurons that fire and wire[19] together are those involving the brain’s survival apparatus. The cortex, “whose job it is to censor inappropriate actions – to exercise the ‘free won’t’”[20] will not develop as it would have done if individuals had experienced secure attachment with a safe, loving, “good enough” primary caregiver.[21]
Fear activates the autonomic nervous system, leading to a fight/flight/freeze, fawn or shutdown response (i.e. dissociation where the brain disconnects from the body to survive a threat). Nervous system awareness may help Probation staff to better understand how an addicted trauma survivor in early recovery can easily relapse due to high levels of interpersonal mistrust, a tiny “window of tolerance”,[22] poor executive functioning, along with impaired attachment/rewards and incentives/motivation brain circuits, all of which were impacted by growing up in an adverse community environment.[23]
In the final article, I explain why Probation practice should return to its relational roots, with an emphasis on co-regulation, cultivating strengths and healing-centred engagement.
Watch also this brief with video highlights on the importance of understanding how stress and distress influence the way we think, feel and act. Produced by The ChildTrauma Academy & Bruce D. Perry, M.D., Ph.D. SevenSlideSeries: State-dependent Functioning.
>>read Part 1 | The importance of nervous system awareness when working with people on Probation
>>read Part 3 | Why a heart-centred approach to Probation Practice is smart
[1] J. Mulcahy, “The Evolution of Punishment and Rehabilitation” (2019) 29(2) Irish Criminal Law Journal 39-49, 43.
[2] J. Mulcahy, Connected Corrections and Corrected Connections: post-release supervision of long sentence male prisoners (UCC, PhD, 2019), available at https://www.researchgate.net/publication/344283849_Connected_Corrections_and_Corrected_Connections_post-release_supervision_of_long-sentence_male_prisoners.
[3] D. Siegel, The Developing Mind: How Relationships and the Brain Interact to Shape Who We
Are (The Guilford Press, 2nd edn, 2015).
[4] B. Perry, “Applying Principles of Neurodevelopment to Clinical Work with Maltreated and Traumatized Children”, Working with Traumatized Youth in Child Welfare, N. Boyd Webb ed. (New York: Gilford Press, 2006) 27-52, 30.
[5] B. Perry, Bonding and Attachment in Maltreated Children Consequences of Emotional Neglect in Childhood (Child Trauma Academy, 2013).
[6] C. Ludy-Dobson & B. Perry (2010), “The Role of Healthy Relational Interactions in Buffering the Impact of Childhood Trauma” in Working with Children to Heal Interpersonal Trauma: The Power of Play, E. Gil ed. (New York: The Guilford Press) 26-43, 39.
[7] J. Mulcahy, Law and Justice interview with Dr Stephen Porges: The Science of Safety, available at https://soundcloud.com/jane-mulcahy/law-and-justice-interview-with-dr-stephen-porges-the-science-of-safety
[8] S. Porges cited in J Mulcahy, ‘The human condition: we are all on a quest for safety’ (2020) 1, online at: https://www.researchgate.net/publication/340309690_The_human_condition_we_are_all_on_a_quest_for_safety
[9] N. Friedman, ‘Eugene Gendlin’s Approach to Psychotherapy: An Awareness of “Experiencing”Annals’ (2004) 23-25 online at: http://previous.focusing.org/pdf/friedman_gendlin_annals.pdf
[10] Child Trauma Academy Channel (2014), SevenSlideSeries: State-dependent Functioning at https://www.youtube.com/watch?v=1uCn7VX6BPQ
[11] D. Andrews & J. Bonta, the Psychology of Criminal Conduct, 2nd ed. (Cincinnati: Andersen Publishing, 1998) 197.
[12] E. Hambrick et al., “Beyond the ACE score: Examining relationships between timing of developmental adversity, relational health and developmental outcomes in children” (2019) 33(3) Archives of Psychiatric Nursing 238-247.
[13] B. Perry & M. Szalavitz, The Boy Who Was Raised as a Dog, 3rd ed. (New York: Basic Books, 2017).
[14] M. Main & E. Hesse, “Parents’ unresolved traumatic experiences are related to infant “disorganized attachment status: Is frightened and/or frightening parental behavior the linking mechanism?” Attachment in the preschool years, M. Greenberg et al. eds., Chicago: Chicago University Press, 1990) 161-182.
[15] Department of Children and Youth Affairs, Lifting the Lid on Greentown – Why we should be concerned about the influence criminal networks have on children’s offending behaviour in Ireland (Dublin: Government Publications, 2016) 40 & 46.
[16] M. Szalavitz & B. Perry, Born for Love: Why Empathy Is Essential-and Endangered (New York: Harper Collins, 2010), Chapter 6.
[17] B. Perry & D. Pollard, “Altered brain development following global neglect in early childhood. Society For Neuroscience: Proceedings from Annual Meeting, New Orleans, 1997.
[18] Hambrick, note 12 above, 239.
[19] See J. Calbet, “Hebb’s rule with an analogy. Psychology and neuroscience” 14 March 2018, available at https://neuroquotient.com/en/pshychology-and-neuroscience-hebb-principle-rule/
[20] G. Maté, In the Realm of Hungry Ghosts: Close Encounters with Addiction (London: Vermillion, 2018), at 292-3.
[21] D. Winnicott, Playing and Reality (London: Tavistock/Routledge, 1971) 7.
[22] Siegel, above n. 3, 281-286.
[23] W. Ellis & W. Dietz, “A New Framework for Addressing Adverse Childhood and Community Experiences: The Building Community Resilience Model” (2017) 17 (7S) Acad Pediatr, S86-S93.

Related News
Keep up to date with the latest developments, stories, and updates on probation from across Europe and beyond. Find relevant news and insights shaping the field today.
New

Overcrowding and Netwidening
Call for nominations Joint Expert Group on Prison Overcrowding and Probation Netwidening (EuroPris & CEP)
09/06/2026
For a new expert group starting in 2026 we are looking for 8 experts (4 from CEP, 4 from EuroPris) interested to join the Joint Expert Group on Prison Overcrowding and Probation Netwidening run in cooperation between CEP and EuroPris.
Recap

Prison, Probation in Europe
CEP at the 31st Council of Europe Conference of Directors of Prison and Probation Services
08/06/2026
CEP participated in the 31st Council of Europe Conference of Directors of Prison and Probation Services (CDPPS), held in Valletta, Malta, on 3–4 June 2026.
New

Caseload and workload
Guidelines on Caseload and Workload
08/06/2026
CEP Expert Group on Caseload and Workload is proud announce the publication of the Guidelines on Caseload and Workload.
Recap

Prison, Probation in Europe
CEP at the 15th Annual General Meeting of EuroPris
04/06/2026
On 2 June 2026, Jana Špero Kamenjarin, Secretary General CEP, represented CEP at the 15th Annual General Meeting(AGM) of EuroPris in Valletta, hosted by the Maltese Correctional Services Agency.
Recap

Caseload and workload
Recap: Workshop on Caseload and Workload
28/05/2026
On 27 and 28 May 2026, Bucharest hosted the CEP Workshop on Caseload and Workload: Supporting Sustainable Probation Through the Human Dimension. With 40 participants representing 18 European jurisdictions, as well as delegates from South Korea, the workshop offered opportunities to exchange knowledge and develop strategies to manage the increasing caseload and workload in probation. Designed as an interactive space, it provided participants – practitioners, managers, researchers and experts – with reflections on current pressures within probation services and it explored practical, evidence‑informed solutions from across Europe.
Recap

Caseload and workload
Recap: Expert group on Caseload and Workload
28/05/2026
On Tuesday 26 May 2026 CEP Expert Group on Caseload and Workload gathered in Bucharest, Romania, for its annual face-to-face meeting, held ahead of the Workshop on Caseload and Workload: Supporting Sustainable Probation Through the Human Dimension. Hosted by the National Probation Directorate, Ministry of Justice, Romania, the meeting was opened by the Deputy Director Diana Mustatea and CEP Secretary General Jana Špero Kamenjarin. They both stressed the importance and relevance of the topic in supporting effective and sustainable approaches to caseload and workload management, contributing to improved outcomes for both staff and service delivery.
Subscribe to our bi-monthly email newsletter!
"*" indicates required fields
- Keep up to date with important probation developments and insights.

